Bariatric Surgery Procedures
Weight-loss, or bariatric, surgery helps you lose weight and lowers your risk of medical problems associated with obesity.
Bariatric surgery contributes to weight loss in two main ways:
- Restriction. Surgery is used to physically limit the amount of food the stomach can hold, which limits the number of calories you can eat
- Malabsorption. Surgery is used to shorten or bypass part of the small intestine, which reduces the amount of calories and nutrients the body absorbs.
Learn about your different options between the weight-loss surgeries, complete with video animations.
Mini-Gastric Bypass
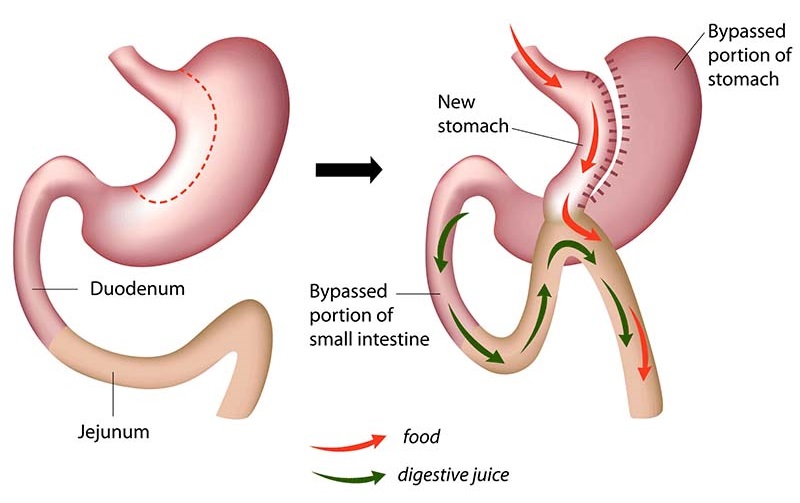
The mini-gastric bypass was developed to reduce operating time, simplify the procedure and reduce complications compared to gastric bypass surgery.
Recent studies show that compared to gastric bypass surgery, mini-gastric bypass reduces operating time, may lead to similar weight loss (some studies show that mini-gastric bypass may actually produce more weight loss), and reduce overall complication rates.
Benefits compared to gastric bypass
- Shorter operation time
- Less re-routing of the intestines
- One fewer anastomosis (connection of intestines), which in theory means less chance of a complication.
- Technically easier for the surgeon
- Similar weight loss and recovery to gastric bypass
Additional risks compared to gastric bypass
- Severe acid-reflux. Because the pouch is small and the remainder of the stomach is still connected to the intestines. It is possible for gastric juices to travel down the intestines and into the new pouch
Gastric Bypass
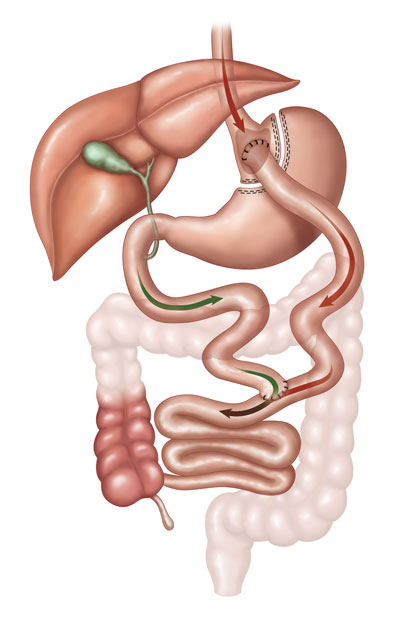
The Roux-en-Y gastric bypass surgery reduces the amount of food that can be eaten due to the smaller stomach pouch. Food is also restricted so that it bypasses most of the stomach and the first section of small intestine (duodenum). Food flows directly into the middle section of the small intestine (jejunum), limiting absorption of calories.
Advantages
- Produces significant long-term weight loss (60 to 80 percent excess weight loss)
- Restricts the amount of food that can be consumed
- May lead to conditions that increase energy expenditure
- Produces favorable changes in gut hormones that reduce appetite and enhance satiety
- Typical maintenance of >50% excess weight loss
Disadvantages
- Is technically a more complex operation than the Adjustable Gastric Banding or Sleeve Gastrectomy and potentially could result in greater complication rates
- Can lead to long-term vitamin/mineral deficiencies particularly deficits in vitamin B12, iron, calcium, and folate
- Generally has a longer hospital stay than the Adjustable Gastric Banding
- Requires adherence to dietary recommendations, life-long vitamin/mineral supplementation, and follow-up compliance
Sleeve Gastrectomy
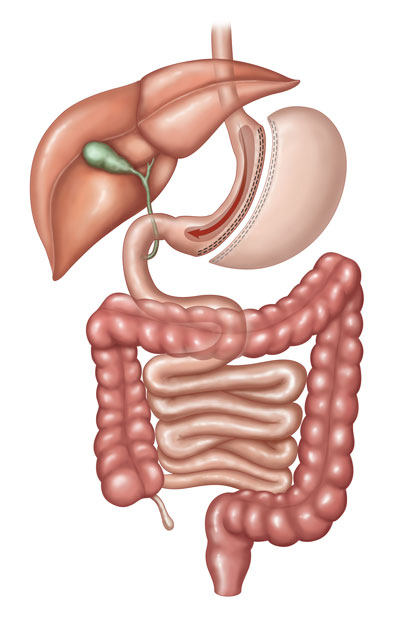
In a sleeve gastrectomy, part of the stomach is separated and removed from the body. The remaining section of the stomach is formed into a tube-like structure. This smaller stomach cannot hold as much food. It also produces less of the appetite-regulating hormone ghrelin, which may lessen your desire to eat. However, sleeve gastrectomy does not affect the absorption of calories and nutrients in the intestines.
Advantages
- Restricts the amount of food the stomach can hold
- Induces rapid and significant weight loss that comparative studies find is similar to that of the Roux-en-Y gastric bypass. Weight loss of >50% for 3-5+ year data, and weight loss comparable to that of the bypass with maintenance of >50%
- Requires no foreign objects (as in Adjustable Gastric Banding), and no bypass or re-routing of the food stream (as in Gastric Bypass)
- Involves a relatively short hospital stay of approximately 2 days
- Causes favorable changes in gut hormones that suppress hunger, reduce appetite and improve satiety
Disadvantages
- Is a non-reversible procedure
- Has the potential for long-term vitamin deficiencies
- Has a higher early complication rate than adjustable gastric band
Adjustable Gastric Band
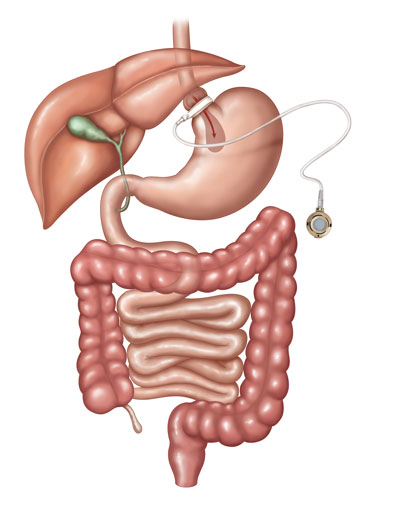
In the adjustable laparoscopic gastric banding procedure, a band containing an inflatable balloon is placed around the upper part of the stomach and fixed in place. This creates a small stomach pouch above the band with a very narrow opening to the rest of the stomach.
A port is then placed under the skin of the abdomen. A tube connects the port to the band. By injecting or removing fluid through the port, the balloon can be inflated or deflated to adjust the size of the band. Gastric banding restricts the amount of food that your stomach can hold, so you feel full sooner, but it doesn't reduce the absorption of calories and nutrients.
Advantages
- Reduces the amount of food the stomach can hold
- Induces excess weight loss of approximately 40 - 50 percent
- Involves no cutting of the stomach or rerouting of the intestines
- Requires a shorter hospital stay, usually less than 24 hours, with some centers discharging the patient the same day as surgery
- Is reversible and adjustable
- Has the lowest rate of early postoperative complications and mortality among the approved bariatric procedures
- Has the lowest risk for vitamin/mineral deficiencies
Disadvantages
- Slower and less early weight loss than other surgical procedures
- Greater percentage of patients failing to lose at least 50 percent of excess body weight compared to the other surgeries commonly performed
- Requires a foreign device to remain in the body
- Can result in possible band slippage or band erosion into the stomach in a small percentage of patients
- Can have mechanical problems with the band, tube or port in a small percentage of patients
- Can result in dilation of the esophagus if the patient overeats
- Requires strict adherence to the postoperative diet and to postoperative follow-up visits
- Highest rate of re-operation
Gastric Balloon
While Gastric Balloon is not an invasive surgical operation, it is a temporary solution for weight-loss if you're overweight or obese.
A saline-filled silicone balloon is placed in your stomach, which helps you lose weight by limiting how much you can eat. It also makes you feel fuller faster.
Gastric Balloon is usually an option if you have body mass index (BMI) between 30 and 40. Intragastric balloons aren't the right choice for everyone who is overweight. A screening process will help your doctor see if the procedure might be beneficial for you.
Advantages
- Loss of about 10 to 15 percent of body weight is typical during the six months following intragastric balloon placement.
- Resolve conditions often related to obesity such as Type 2 diabetes, heart disease, high blood pressure, severe sleep apnea, etc.
Risks
- Pain and nausea affect about one-third of people soon after insertion of an intragastric balloon. However, these symptoms usually only last for a few days after balloon placement. And they can be treated with oral medication.
- Serious risks after intragastric balloon placement and removal are rare. It's possible that the balloon could deflate. If the balloon deflates, there's also a risk that it could move through your digestive system. This can cause a blockage that may require a further procedure.